|
Since entering college, I have changed an indescribable amount. When starting in the program as well as school I was extremely insecure and was not sure how I needed to study in order to succeed. After my first semester in the program I spent a semester in remediation, which at the time was the worst possible thing that happened to me. However, looking back at it now it was the best possible thing. I figured out how I learned, failing helped me succeed in the rest of my college career. I know I am not the same person that entered college, maybe physically but mentally am incomparable.
I have done many things in the last three years that I never would have thought I ever would have done. First, in the spring of my junior year I presented in a breakout session on Ampersand day about research myself and Laura had worked very hard on. Presenting in front of fifty people was something I never would have thought I would have done but pushed me outside my box and forced me to become more confident. Second, in the spring of my senior year I traveled with Kings College to London, England with over fifty other Athletic Training students from around the country. That experience was one that I will forever treasure because I met some awesome new friends as well as new knowledge that I will be able to apply to my work. Third, in the spring of my senior year I presented in the student showcase ALONE in front of over 300 people on Ampersand day about traveling to London. This experience was one I never saw myself doing, entering college I was never comfortable in front of a large group of people and now I am able to do it with some ease. Before presenting I thought I was going to throw up but when I got on stage I felt a lot better and was able to do my presentation with ease. One thing I am most thankful for are my preceptors, friends and professors who encouraged me to be the person I am today. Melissa first pushed me and instructed me on how to be a great AT. Chaypin, Joe and Alex allowing me to be on my own and make decisions throughout rehabs and evaluations. D.C. for making me take the big leap back into the program. Beth for yelling at me and making me gain confidence. Lastly, all the friends I have made in the program, Sam and Colin for being my buddies through the program. And Sam for the countless hours we studied for exit exams. After graduation I will be heading to Puerto Rico to be an assistant AT for the Puerto Rican Collegiate League. I am very excited for the opportunity and am excited to see where it takes me after returning. I included one of the first pictures I took entering college and one of my senior pictures I took only a couple weeks ago. I was added a couple pictures from Ampersand Day!
0 Comments
My skills communicating with physicians and other healthcare providers has grown a lot since starting this school year. Experiencing the Ortho clinic multiple times over the last year and having Dr. Handy rotations has help tremendously with that. While doing the Ortho clinics I had to take the do an evaluation of the patient then communicate it back to Dr. Hannula to give him the proper background about the injury. After the clinic was completed, I also had to do claim forms, new patient forms, type up demographics, and scanning in claim forms to Melissa or faxing new forms and demographics to Dr. Hannula’s office. Then after everything was sent, I called his office to make appointments for the patients. I had to communicate with his office and with my patient in order to smoothly schedule appointments. Calling his office and setting up appointments was a new experience for me, which will help me a lot in the future in case I have to set up appointments for my athletes. In order to communicate with his office appropriately there were many steps that needed to be done prior to the visit, the demographics and new patient forms. As well as on our side, claim forms needed to be scanned in, in order to athletes to go see Dr. Hannula in office or have X-rays or MRI’s done.
While rotating with Dr. Handy, I learned how important communications is with other healthcare providers for refers or even with other doctors in the office. While I was with Dr. Handy there were many times when he needed to refer a patient to a specialist and was able to do it without a thought. Dr. Handy has relationships with other specialists around the area and he is able to communicate to his patients who they need to go see in order to get the proper care. I believe that one of the main reasons’ communication needs to be so strong between an AT and a physician is to have trust in the AT as well as the other way around. Having trust in each other will allow for a smooth recovery process of the patient, the physician to have trust in the AT so they believe they are following proper protocol as well as the athlete to trust that the AT understands what they are doing throughout the process. Communication between the athlete, AT and physician is necessary in case of any changes for a rehab and to follow the post-surgical protocol for optimal success of the athlete. This weekend was very crazy! As a senior class we had the opportunity to experience the AAU national wrestling tournament. There were 38 elementary aged teams from all over the nation. We not only did experience the tournament but also leading up to the tournament we had to do the administrative part. We created a Policy’s and Procedures manual as well as created evaluation sheets and a contact for the event.
The tournament started on Friday night, we are drove down and were able to get there before the tournament started to look around and assess the situation. The tournament started fast, and the rush did not stop until it was over. There were 8 matts in the main gym and the 2 additional matts in a practice gym. We had a great system going, in the middle of the eight matts in the main gym were the tables and workers, there were four corners. Four of us were in the main gym and the other two were in the practice gym. It worked out so well, someone was in each corner scanning three matts at the time but sharing two of the three mats that were being scanned, so it someone had to run out there was always someone else there. To start off the tournament Sam and I were in the practice gym and one little boy got hit in the nose and started bleeding, but it was no normal nose bleed, it would not stop. So, Sam tried and tried to stop the bleeding, but it was too much for one person to handle. I tried putting skin lube in his nose, but nothing was working. One of the coaching while I was helping was trying to tell me what to do and to fold the nose plug and put it up his nose, his nose was not very big, and it folded would not fit or stay in. I tried and tried to explain to him we could not put the plug in his nose until the bleeding slowed down. The bleeding started coming out of his mouth and was dripping out of his nose. We finally got the bleeding to slow down with 10 seconds left on the clock, we stopped blood time then started to clean the boy, it was everywhere it felt like we had been working on this boy for 30 minutes. We got a nose plug in, but the coaches were worried it would come out, he only had 14 seconds left and they told us to tape it to his head, so we put gauze and powerflex and taped it to his head. So, we did and 4 seconds into the match his nose started bleeding again and blood time ran out and the boy was disqualified. Which brings me to my strengths and weaknesses, I handled that situation well with the boy but not with the coaches I should have asked the coaches to step away and let us try to stop the bleeding. However, when an older man is breathing down your back and trying to tell you demandingly what to do it’s hard to do. If I am ever in a position like that again I know now how to handle it appropriately. I started off this week on Tuesday with a very large accomplishment, taking my Board of Certification exam. I was a very difficult exam but am hoping I did well on the exam.
We were supposed to start our clinical appraisal this week, however, were unable to do so. Brianne had us write down topics that interested us and she would assign the papers that she wanted us to appraise. We have spent a lot of our time in the past two weeks looking at the checklists and scales at are used during the appraisal process. On Friday we looked at the PEDRO scale. We went through an article and evaluated if it checked off on the PEDRO scale. The PEDRO scale was developed by the Physiotherapy Evidence Database to determine the quality of clinical trials. The checklist consists of 10 yes or no questions. While working on the checklist I did get confused with some of what the questions were asking. The article had to spell it out if it was a yes or a no, it either had it or it did not. We were put into pars and worked on the checklist together. I was assigned to work with Katie, we were only given about 10 minutes to read the article, which was not enough it. While Katie and I were going down the checklist we really realized we had no clue what the checklist was even asking on some of the questions. We felt like we were thrown in the dark. We ended class on Wednesday evaluating and would finish and discuss the checklist on Friday with our answers. On Friday while we were discussing we agreed that the article either was a 5 or 6. While discussing the answers some of us were confused how they were no’s when we had yeses. The questions on the list are not explanatory so understanding why something was no over yes was a bit difficult. Last semester I found an interest in hypertrophic cardiomyopathy, so this semester I was hoping in do more research on the illness as it compares to athlete’s heart. Two very similar conditions, with two different out comes. I did research on the gold standard test to confirm the illness, but now I would like to know more about the two illnesses compared to one another. I would really like to learn more about athlete’s heart and how it resolves itself after disqualifying from activity. I have improved on all of my goals that I set at the beginning of the semester: improving domain 5, improving domain 4, and improving domain 2. I intended to improve all of the domains so that I was able to pass a practice exam, so I was able to sit for my BOC in the March/ April window. Which I did and will be sitting for my exam in a week and a half.
On all of the practice exams my lowest grades were in the three domains I chose at the beginning. My lowest scores across all of the practice exams were in healthcare administration. I decided that to increase my score I needed to review budgeting techniques along with athletic training principle terminology. My second lowest scores were in therapeutic innervation, I knew that I needed to improve on that domain because it contains the majority of the therapy knowledge and weighs the most on the exam. I was able to do a lot of practice questions this week with Alex, he gave me some scenarios from emergency care as well as some terminology. A large section in domain five that I struggled with was understanding negligence terms. I understood the definitions but could not keep the terms straight. When I was practicing with Alex, he was giving me examples of each term and I was able to understand a little bit better. I decided there are some things based on my notes from the last practice BOC that are still very “muddy” to me due to the lack of knowledge. I struggled a lot with the nutrition aspect of domain 4. I made a chart of the vitamins and minerals with their functions and how it would appear if an individual with lacking the vitamin or mineral. Domain 4 also addresses modalities and I understand how to use the modalities but was not very sure why and how the modality was working on the body. Some of the electrical stimulations and ultrasound were still a bit confusing to me, but after some direct studying of those particular modalities I was able to understand a bit better and apply it in the clinic while during treatments. This week we, the athletic training program, were able to meet with Congressman Morgan Griffith and discuss with him why we are healthcare and could save the country a lot of money in the medical field. We also discussed the problems with opioids in the country, discussing how we could eliminate the use of opioids in the younger population. Congressman Griffith is a graduate of Emory & Henry and he really enjoyed being back at the school. We walked him through the depot showing him how much change has gone into the school then walked over to the king center to show him the clinic and one of his favorite spots on campus, the swimming pool. I really enjoyed meeting him and hearing lots of his stories from when he was a student at E&H. I have included a picture of the program with Congressman Griffith. This year’s National Athletic Training Month slogan is: “ATs ae Health Care.” This slogan means a lot to the athletic training field because athletic training is not seen by the public as a part of the medical field. Many people do not even understand what athletic training is and what ATs really do. Many people think athletic trainers are the “glorified water boys” on the side of the field in the NFL games. Some people even address athletic trainers the completely wrong way. Some may say “trainers” thinking that we are the ones that help lift and get people into shape. No, those are personal trainers or strength and conditioning coaches.
Wikipedia states, “An athletic trainer is a certified and licensed health care professional who practices in the field of sports medicine. Athletic Training has been recognized by the American Medical Association (AMA) as an allied health care professional since 1990.” In 1990 athletic training was finally recognized as a medical profession many people still lack the proper knowledge on what an athletic trainer truly is. To obtain an athletic training degree someone must have a bachelor’s in Athletic training but however now is transitioning into a master’s program, pass the Board of Certification (BOC) exam and follow the proper criteria for their state, which may include a license to practice. The National Athletic Trainers’ Association (NATA) states, “Athletic training is practiced by athletic trainers, health care professionals who collaborate with physicians to optimize activity and quality of life for patients both of the physically active and sedentary population. Athletic training encompasses the prevention, diagnosis, and intervention of emergency, acute and chronic medical conditions involving impairment, functional limitations and disabilities." Many people, unless having worked with an athletic trainer, do not understand how much work, time, and emotion going into the teams and athletes’ that we work with. As an athletic training student at Emory & Henry College I have learned many skills that will help me succeed in the future as an athletic trainer. I have always learned over the last few years how many people truly do not understand what an athletic trainer is, so in the future I hope to educate students and motivate them to pursue a degree which they are passionate about. This week was a very slow week after the rugby team’s game this past weekend the coach decided to give the team the week off before they leave to go to Savannah. So, I was not able to do much rehab with my rugby players. I did however get to see two of my cheerleaders, the two who fractured bones. Joe and I decided to start rehab with them focusing on the joints above and below the cast. On Monday I started rehab with the cheerleader who fractured her scaphoid and radius. While tumbling she went to twist to go into a back-handspring and fell improperly on her wrist. I decided it was very important while she was in the cast to keep the fingers moving. So, introduced her to flexion and extension with bands, spreading out putty, and the web. I had her do three sets of ten for each exercise. The day after she fractured her scaphoid and radius another cheerleader was dropped from the top of a pyramid, she dislocation her shoulder and fractured her proximal radius. She was casted four days later. I will approach her with the same rehab as the other cheerleader.
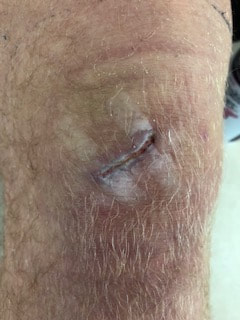
I experienced something I had never done before. While with Alex an athlete came in and Alex instructed me to do an ultrasound. But he went on telling me how to do it, I was a bit confused at first, he was talking about medicine and how to place it. I just stood there and looked at him, then he said phonophoresis, it then made since. I hadn’t ever done phonophoresis, we had talked about it in class but very practiced. So, this athlete has patella tendinitis and his PT prescribed him Voltaren gel (Diclofenac Sodium Gel). On the prescription it describes everything from the amount to the parameters that is needed for the procedure. For his treatment he requested 4 ounces on 100% and 1.2 intensity. Alex told me to do four lines about an inch each around the knee then add the ultrasound gel in the middle. The prescription did not come with a treatment time so after the calculation the treatment time was about 6 minutes. After the treatment he was able to complete exercises without much pain. On Wednesday, my rugby player came in. I have attached pictures, the first one is from right after the game and the second one is from Wednesday after taking off the bandage. I was very impressed with how great it was looking and how it closed up nicely. Joe and I decided that laser would be a good treatment for him because the laser promotes healing. Joe decided to put a piece of plastic over top of the wound and then do the laser on that to prevent from exposure. We have been looking at other ways to speed up his healing to get him back to the field as fast as possible. I was a little worried with how moist the wound was, but Joe and I decided to keep it covered for one more day to let to scab heal a little more. This weekend was full of excitement. The weekend started with a busy Saturday, we hosted Virginia Tech and Pitt’s women’s rugby teams. The day was supposed to be full of games. Emory & Henry women’s and men’s vs. VMI women’s and men’s teams. However, our women were unable to play because VMI women did not travel. A full rugby game is 15 players from each team on the field and two 40 minute halves. During the first half of the women’s game one of the Pitt players went down then tried to continue running after. However, she was in too much pain to continue. She was a very small girl, very skinny, it was a very cold which made it very hard to warm up. She took a cleat to the leg and had the start of a nice bruise on her quad. When I was examining her, I could tell that she was extremely cold and unable to really warm up and prevent from her legs from getting stiff, so she decided to pull herself from the game. During the second half another player from Pitt went down hitting her head, but as I started to approach her, she jumped up and continued playing. I keep a close eye of her and every couple minutes she would touch her head, but would not come out. After the game she came up to me and explained she had a headache and felt like she was in a daze but did not want to come off the field during the game. I looked at her eyes and there was some nystagmus. I told her to avoid anything that worsens symptoms, so if light was bothering her to stay away from her phone and rest.
Earlier in the week I was able to take out one of my rugby players stitches from a rugby match two weeks prior. The wound was healing nicely, and the scab looked great, so Joe and I felt good about take out his stitches. So, I was able to remove his stitches without a problem and have him practice Thursday. I was hesitant to having him play in the game Saturday, but he had sat out for two weeks and was ready to get going again. I padded him up really good and keep it clean, however during the first half I noticed blood coming through the gauze, I checked on him, but he claimed he was okay and kept playing. Then about half way through the first half a VMI player come up to me complaining of posterior shoulder pain, while I accessed range of motion his right arm was only able to get about half way compared bilaterally and strength was about the same. He was pretty weak and very tender on the posterior shoulder muscles. I decided a posterior subluxation while playing most likely happened. I created a sling with his sweatpants and put ice on his shoulder. I checked on him a couple times throughout the game, but he seemed be doing well. Near the end of the second half my player went down and when getting up seemed to be in pain on his right shoulder and had a large amount of blood in the gauze on his knee now. I ran up to him and as I was walking up the game ended, I peeled off half of the gauze and noticed the scab was non-existent and the cut was completely reopened. Joe and I started to go through options in our heads and then the coach said his friend that is an anesthesiologist was at the game. We walked over to him and he confirmed the he cannot be re-sutured so keep it clean, antibiotic ointment, covered, butterflied and allow it to heal on its own. On Sunday I passed my practice BOC exam, so I will be able to sit in the March/April window! For a future job I know that building a resume can be the most important thing to do to look appealing for future employers. Coming from a bachelor’s degree when the athletic training degree is now transitioning into a master’s programs in going to be a challenge for what I wish to go into. But nothing looks better than the experience and who you know. While I was in London, I talked to many of the athletic trainers for professional baseball teams as well as the president for PBATS and they explained to me that they want to see that you have had the hands-on experience and thy want to really know what you can do. I understand that I will not start off in the MLB but have to work my way up from the minor league. Mark O’Neal also told me that once they see what you can do, if they get a call from a team needed an athletic trainer, they will refer you themselves.
I would like to further my education and continue on to receive my DAT, however I would like to get my foot in the door first and work in the field. I also did my second Ortho clinic of the semester. I was able to present three patients to Dr. Hannula. The first patient, a cross country/ track runner, who has a deformity on their medial shin. I have worked with this athlete before and knew they said when massaging it, it will go away for a little while and decreasing the stress load while running. Dr. Hannula looked at it and was confused by it, thinking possibly a cyst but needing x-rays and an MRI to rule in the injury. So, I was able to fill a claim form and instruct the patient to fill out new patient paperwork. The second patient, a rugby player, during the tournament Saturday dislocated their shoulder and was able to reduce it, this was their first time dislocating their shoulder. Dr. Hannula explained that once someone experiences a dislocation 50% will experience another dislocation. He said that right now there is no need to do any imaging just strengthen the shoulder. I was able to put the evaluation into ATS but no additional information was necessary unless a dislocation occurs again. The third patient I saw was a follow-up, this patient is a rugby player who is recovering from surgery after a tib-fib dislocation, fib fracture and anterior compartment syndrome. Dr. Hannula encouraged them to start bearing weight and work of ROM. They needed additional imaging along the way to conform that healing was adequate, so I needed to complete a claim form along with USA rugby forms to cover extra costs. I learned a lot of new things this week just from Monday, including how to use a fax machine. It is extremely important for a patient to trust their AT for optimal healing and recovery because they will do what is necessary that the AT says to recover. First an AT must build trust with their athletes. I believe this is done by becoming friends with the athletes. I learned how important this is from Chaypin while working with women’s soccer. At the start of the session I was new to them, no one really know me that well and therefore did not trust me yet. I became very close with the soccer team in the first two weeks of preseason, building good friendships with the players. With friendships came trust. Once the session got going, we had a very hard session with injury after injury and rehab after rehab, trust was necessary. They needed to trust that we were going to be able to get them back on the field and in their prime. Chaypin allowed me to do a lot with each of the players, allowing her to also build trust in me.
When an athlete does not trust their AT they may skip rehab or skip going into the clinic to be evaluated or get treatment. When trust is not there between the AT and the athlete it may expose them to more injury. I believe that trust is the most important part of any relationship. I had a very exciting week with many rehabs that I have never experienced before from an athlete that is unable to lay supine because of a 6-8 inch scar on his bad from back surgery in the last year, to a rugby player who is recovering from a compound fracture of his tibia and fibula and anterior compartment syndrome 9 weeks out from surgery. I was also able to complete many evaluations the most exciting being an athlete with no known underlying conditions suffered seizure like symptoms, out of body experience, numbness in the extremities, dizziness, and inability to see or communicate, while running during a workout. He stopped and sat down, he was a completely different person compared to his normal self. Once he stopped running and sat down, his symptoms were still consistent, however about an hour later his symptoms started to subside. upon entering the clinic, he had nystagmus of his right eye, a pulse oz. of 96%, BP of 138/ 93, 135/93, 133/83, and a pulse of 105 at this point he had not run since he first stopped. We then had him complete a PRO of feeling. It started to raise questions as to why this was happening, if it had something to do with sleep, food, or the weather. I was also able to experience my first rugby game, one of the most exciting things I have experienced as an athletic training student. I love emergency care and that’s what I did more than anything on Saturday. I was on my toes the whole day from tons of turf burn to shoulder dislocation. The most exciting part of the day was while my back was to the field. I was doing a knee evaluation when all of the sudden a heard a giant thud, I turned around and saw a player lying on the ground not moving. I immediately stood up and ran over to the player. Joe secured c-spine and I asked the player if he could move his toes and fingers and he did I checked pulses in wrists and ankles, both good. He then started to move his legs and he knew that no life-threating injuries. We then decided that the player rolled over and hit his knee on the bench. I think more than anything he was scared and just had a contusion on his knee. On my first BOC practice exam junior year on April 8, 2018 my scores reflected from the classes I had taken, with my lowest scores in domains 4 and 5. Domains 1 through 3 were all 80% or above with a distributed total average of 69.3%. At that point, I knew where I really needed to focus and also needed to complete another class, organization and administration. I also really needed to work more in domain 4, therapeutic intervention, it has been my lowest score consistently the two times we have taken practice exams. Domain 4 weighs the heaviest on the exam and contains the most content with pharmacology, general illnesses and injuries, therapeutic exercise, modalities, and manual techniques.
On my second BOC practice exam on January 22, 2019 my scores in domains 3 through 5 increased by 4-6% however domain 1 and 2 decreased by 10-12% which took my distributed average down by 2% sadly. I took that exam two days after returning from London and while taking the exam felt pretty bad about it. I had many things to look over again and some unfamiliar terminology, so I am grateful for having theses exams in preparations for the BOC in March. I did however meet “possible strength” on domain 3, emergency care. There are still many things that I need to review as well as study a lot more. I am starting to get on a study plan to review all of my weaknesses. On my third BOC practice exam on February 3, 2019 I felt good going through the exam but did not end that way. I had a distributed average of 61.7% the only domain that I did not go down in was domain 5. I also went down 24% in domain 3, emergency care, which was very upsetting because I did not feel that I did bad during that exam. I have always been prepared for an injury during clinical experience. However, this week was a very bad week. I have had a hard week with being confident with myself in the clinic and as an athletic training student, so all I can do now is just study and move forward and succeed on the next exam. This week I was able to experience my first ortho clinic of the semester. I was able get the history of three athletes, a soccer player, a cheerleader, and a rugby/ thrower/ cheerleader. They all had very different injuries. First the soccer player who has very rounded shoulders and tendinitis with weakness in the upper back. Dr. Hannula recommended strengthening the upper back and taking alive two times a day. The second patient, the rugby/ thrower/ cheerleader, tore their ACL in the past and while doing box jumps experienced a pop on the medial side of the knee, he sent the patient for imaging the previous week. They athlete’s ACL had scared into the PCL and had tears in both menisci, however with no difficulty or pain Dr. Hannula recommended to just work on strengthening the knee. The third patient, the cheerleader, had been dropped on their neck in practice and was referred to the ER and was diagnosed with a pinched nerve in their neck. Following up with Dr. Hannula he did not agree with that diagnoses but thought they had subluxed or dislocated their shoulder. He recommended strengthening the shoulder and not too much the shoulder past the body’s midline. The most interesting case was with a football player that two hours earlier was doing hang cleans and biceps just popped. Dr. Hannula supinated and pronated the hand and attempted to hook the distal biceps tendon which was extremely positive, nothing was even there. An extreme deformity of the biceps was there as well. The athlete was in extreme pain but has had experience with many ruptures before. Hannula decided that no farther testing was needed and diagnosed a distal biceps tendon rupture. After all the patients left, I asked Dr. Hannula about biceps ruptures and how common they were in collegiate athletes and he said he had only ever seen two cases of biceps ruptures, both this year. I have experienced both of the diagnostic processes with Dr. Hannula. My gender I believe will be the biggest challenge in my career. I am applying for the PBATS, professional baseball athletic training society, internship for this summer with the Minor League and the MLB players. I know that many guys have a difficult time talking to a woman about injuries, especially injuries near or in the groin, without trust and knowledge that that woman is a good Athletic Training. Before the PBATS internship I am privileged enough to go down to Puerto Rico and work in the Puerto Rico Collegiate League with 250-300 baseball players from 17-22 years of age. I am extremely excited to be able to work with so many players and prove myself to not only the boys but also the coaching staff. My dream is to work in professional baseball because it is a challenge to me and puts me outside of my comfort zone with the shoulder. I have decided when I am put outside of my comfort zone that I am forced to be a better AT and think outside of the box. The shoulder is a very interesting complex to me with so many different muscles that can be involved. This summer while working in Puerto Rico I wish I create a warm-up and cool-down program that when properly done will strengthen and prevent shoulder injuries in the players future careers.
Another challenge I face in the field is my size and age. Most baseball players tower over me so some my doubt that I cannot stretch or properly evaluate them because I cannot hold them. However, some of them may be very large but I can use cheats to be able to properly evaluate and or stretch them. Some people think I am very younger when first looking at me and some cases I may be, professional baseball ATs have spent many years in the field and worked their way up, which I am prepared to do. Lastly, a challenge I face in everyday life, disabilities I have in school work and learning I do not learn as fast and do not grasp many concepts as fast, but I believe that it is not a weakness, it is a strength. I have failed in the past, and it has forced me to come back stronger and work 100 times harder for what I want to accomplish. Some people doubt my knowledge because of how I look or what they know but I am prepared to prove many people wrong. Although I face many challenges, I am prepared to face them head on, just like all the challenges I have faced in the past. I feel that I have grown a lot this semester, not only with Athletic training but also as a student. This semester I as an athletic training I have not run away from evaluations, something in the past that I would have run away from. Also, in the past I would have looked for a preceptor to help with diagnoses. My feedback from my preceptor was just as a thought. Chaypin said she wouldn’t have been able to make it throughout this semester, which really helped with my confidence. This semester was a little crazy, with injury after injury with women’s soccer, but we made it through. She said that some things I needed to work on were evaluations of the shoulder as well treatment for the shoulder. I have always been very determined to be an extremely organized and determined athletic training student.
As I prepare for the spring semester, I wish to become more proficient with evaluation of the shoulder and diagnosing shoulder injuries. Being with track and field I hope to see many upper injuries with our throwers. This weekend has been a bit crazy, we take our exit exams on Friday and I am currently in D.C. for a family Christmas party and it is down pouring snow for Roanoke all the way back to school and are predicted to get over a foot of snow, so I will not be able to get back to school until Monday afternoon to start studying to my exit. I am very excited for this exit because we get to connect everything together. From the start of sophomore year with learning special tests and about the areas we are dealing with then into junior year connecting the special tests with injuries. Finally this year putting injuries and general illnesses/ conditions with the tests required to diagnose them and finally how to treat them. Without clinical packets this semester, I have had a hard time forcing myself to study throughout the semester. I have stressed myself out a lot this semester about our comprehension exam at the end of this semester. I feel this semester will be the hardest exam for me so far in my career, because the way I have been studying for exams in the past has to change. I completed goals at the beginning of the semester.
My first clinical goal was to complete 20 questions in my BOC prep book per week in preparation to pass my BOC exam in the spring. Over the semester I was working over hard in my book treating is as our clinical packet, however while working in it felt like there were some things I needed to learn and review more. My second clinical goal was to improve domain 4, therapeutic rehab by setting up mock or real injury rehabilitation exercises, two per week. I feel that i have learned a lot in this domain over the semester. I have been completing rehabs for athletes with shoulder, back, knee, and ankle. I have described what exercises are important for them to complete and why. My third clinical goal was to improve on evaluation of the shoulder by performing shoulder evaluation, one every two weeks. With this goal I feel I have improved tremendously and will continue to improve over the next couple months with the conference in January and experiencing with throwing athletes next semester. I have also worked with Alex, my potential preceptor for next semester, on the shoulder with muscles which is what I have struggled with. My last clinical goal was to improve on analyzing athletes’ nutrition habits to treat and/ or prevent injury or illness, by analyzing an athlete, one every two weeks. This goal has been much harder than anticipated, trying to find athletes willing to track all their food. I hope to complete this goal into next semester. This week was my last time experiencinging with a horse show for the semester. Before the show began an athlete who was not competing came up to Chaypin and I and asked if we could look at her ankle. I knew this athlete had previously had ankle difficulty. She had surgery in December of 2017, however was still experiencing some pain in her posterior ankle. She continued to tell me that the surgery done was to tighten the loose tendon of the puronial and reattach it. She had completed three rounds of PT but felt like she was very tight. I began to palpate but found no deformities I tested her ROM and strength which were all excellent compared bilaterally. I made sure to do Kliger’s, Talar tilt, anterior drawer, and bump test, which were all negative. I then discovered she was tight in both calves which was causing her pain. I told her to come in to the clinic Monday and we could begin some treatment to address the tightness. HAPPY THANKSGIVING eat a lot of food!
I believe my strongest domain is emergency/ immediate care. I have not been able to experience many emergency situations, however am always very prepared for them to happen, while clinically experiencing I make sure to formularize myself with locations to all emergency equipment and EAPs in cause of an emergency. While during clinical experience I have explained to my preceptors that I would like for something to go wrong. So, then I am able to get the experience of a true accident before I am an AT myself. We now have access to the simulation lab in Marion, we are able to run codes and experience the true natural of an emergency. I feel that I also understand how emergency situations need to be handled whether it is a C-spine injury or a broken bone. Another domain I ham strong in is evaluation, however am much stronger in the lower body than the upper body. I am very confident with lower extremities because I feel like I have been around them the most since entering the program. I am able to match most injuries just from the mechanism of injury for lower body. However, am not as strong as I would like to be for evaluation of the shoulder and back. The special tests for those areas have been very hard for me to remember and truly understand. I have not experienced many injuries in the sports that use shoulder and upper body. But I feel very confident with wrist and hand, but just lack some knowledge for the shoulder and back. However, hopefully after the conference I am attending in London will help me understand upper evaluation a bit better. One way I can strengthen that weakness is by doing more evaluation for upper extremities, whether they are real or just mock evaluations. My biggest weakness is definitely organization and administration, I am O&A right now, so I am still learning most of the material for that domain. The hardest thing that I am having a hard time understanding are the different types of budgets, what they are, when they are used and how they are used. However, after going through and building our own athletic training room and supplying it I feel that I have a better grasp on things. I am going to work much more in that chapter of my BOC prep book, to strengthen that weakness |







 RSS Feed
RSS Feed
