|
I have improved on all of my goals that I set at the beginning of the semester: improving domain 5, improving domain 4, and improving domain 2. I intended to improve all of the domains so that I was able to pass a practice exam, so I was able to sit for my BOC in the March/ April window. Which I did and will be sitting for my exam in a week and a half.
On all of the practice exams my lowest grades were in the three domains I chose at the beginning. My lowest scores across all of the practice exams were in healthcare administration. I decided that to increase my score I needed to review budgeting techniques along with athletic training principle terminology. My second lowest scores were in therapeutic innervation, I knew that I needed to improve on that domain because it contains the majority of the therapy knowledge and weighs the most on the exam. I was able to do a lot of practice questions this week with Alex, he gave me some scenarios from emergency care as well as some terminology. A large section in domain five that I struggled with was understanding negligence terms. I understood the definitions but could not keep the terms straight. When I was practicing with Alex, he was giving me examples of each term and I was able to understand a little bit better. I decided there are some things based on my notes from the last practice BOC that are still very “muddy” to me due to the lack of knowledge. I struggled a lot with the nutrition aspect of domain 4. I made a chart of the vitamins and minerals with their functions and how it would appear if an individual with lacking the vitamin or mineral. Domain 4 also addresses modalities and I understand how to use the modalities but was not very sure why and how the modality was working on the body. Some of the electrical stimulations and ultrasound were still a bit confusing to me, but after some direct studying of those particular modalities I was able to understand a bit better and apply it in the clinic while during treatments. This week we, the athletic training program, were able to meet with Congressman Morgan Griffith and discuss with him why we are healthcare and could save the country a lot of money in the medical field. We also discussed the problems with opioids in the country, discussing how we could eliminate the use of opioids in the younger population. Congressman Griffith is a graduate of Emory & Henry and he really enjoyed being back at the school. We walked him through the depot showing him how much change has gone into the school then walked over to the king center to show him the clinic and one of his favorite spots on campus, the swimming pool. I really enjoyed meeting him and hearing lots of his stories from when he was a student at E&H. I have included a picture of the program with Congressman Griffith.
0 Comments
This year’s National Athletic Training Month slogan is: “ATs ae Health Care.” This slogan means a lot to the athletic training field because athletic training is not seen by the public as a part of the medical field. Many people do not even understand what athletic training is and what ATs really do. Many people think athletic trainers are the “glorified water boys” on the side of the field in the NFL games. Some people even address athletic trainers the completely wrong way. Some may say “trainers” thinking that we are the ones that help lift and get people into shape. No, those are personal trainers or strength and conditioning coaches.
Wikipedia states, “An athletic trainer is a certified and licensed health care professional who practices in the field of sports medicine. Athletic Training has been recognized by the American Medical Association (AMA) as an allied health care professional since 1990.” In 1990 athletic training was finally recognized as a medical profession many people still lack the proper knowledge on what an athletic trainer truly is. To obtain an athletic training degree someone must have a bachelor’s in Athletic training but however now is transitioning into a master’s program, pass the Board of Certification (BOC) exam and follow the proper criteria for their state, which may include a license to practice. The National Athletic Trainers’ Association (NATA) states, “Athletic training is practiced by athletic trainers, health care professionals who collaborate with physicians to optimize activity and quality of life for patients both of the physically active and sedentary population. Athletic training encompasses the prevention, diagnosis, and intervention of emergency, acute and chronic medical conditions involving impairment, functional limitations and disabilities." Many people, unless having worked with an athletic trainer, do not understand how much work, time, and emotion going into the teams and athletes’ that we work with. As an athletic training student at Emory & Henry College I have learned many skills that will help me succeed in the future as an athletic trainer. I have always learned over the last few years how many people truly do not understand what an athletic trainer is, so in the future I hope to educate students and motivate them to pursue a degree which they are passionate about. This week was a very slow week after the rugby team’s game this past weekend the coach decided to give the team the week off before they leave to go to Savannah. So, I was not able to do much rehab with my rugby players. I did however get to see two of my cheerleaders, the two who fractured bones. Joe and I decided to start rehab with them focusing on the joints above and below the cast. On Monday I started rehab with the cheerleader who fractured her scaphoid and radius. While tumbling she went to twist to go into a back-handspring and fell improperly on her wrist. I decided it was very important while she was in the cast to keep the fingers moving. So, introduced her to flexion and extension with bands, spreading out putty, and the web. I had her do three sets of ten for each exercise. The day after she fractured her scaphoid and radius another cheerleader was dropped from the top of a pyramid, she dislocation her shoulder and fractured her proximal radius. She was casted four days later. I will approach her with the same rehab as the other cheerleader.
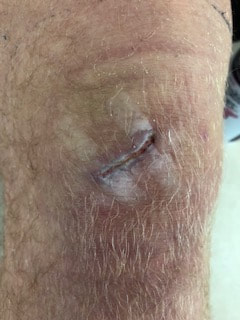
I experienced something I had never done before. While with Alex an athlete came in and Alex instructed me to do an ultrasound. But he went on telling me how to do it, I was a bit confused at first, he was talking about medicine and how to place it. I just stood there and looked at him, then he said phonophoresis, it then made since. I hadn’t ever done phonophoresis, we had talked about it in class but very practiced. So, this athlete has patella tendinitis and his PT prescribed him Voltaren gel (Diclofenac Sodium Gel). On the prescription it describes everything from the amount to the parameters that is needed for the procedure. For his treatment he requested 4 ounces on 100% and 1.2 intensity. Alex told me to do four lines about an inch each around the knee then add the ultrasound gel in the middle. The prescription did not come with a treatment time so after the calculation the treatment time was about 6 minutes. After the treatment he was able to complete exercises without much pain. On Wednesday, my rugby player came in. I have attached pictures, the first one is from right after the game and the second one is from Wednesday after taking off the bandage. I was very impressed with how great it was looking and how it closed up nicely. Joe and I decided that laser would be a good treatment for him because the laser promotes healing. Joe decided to put a piece of plastic over top of the wound and then do the laser on that to prevent from exposure. We have been looking at other ways to speed up his healing to get him back to the field as fast as possible. I was a little worried with how moist the wound was, but Joe and I decided to keep it covered for one more day to let to scab heal a little more. This weekend was full of excitement. The weekend started with a busy Saturday, we hosted Virginia Tech and Pitt’s women’s rugby teams. The day was supposed to be full of games. Emory & Henry women’s and men’s vs. VMI women’s and men’s teams. However, our women were unable to play because VMI women did not travel. A full rugby game is 15 players from each team on the field and two 40 minute halves. During the first half of the women’s game one of the Pitt players went down then tried to continue running after. However, she was in too much pain to continue. She was a very small girl, very skinny, it was a very cold which made it very hard to warm up. She took a cleat to the leg and had the start of a nice bruise on her quad. When I was examining her, I could tell that she was extremely cold and unable to really warm up and prevent from her legs from getting stiff, so she decided to pull herself from the game. During the second half another player from Pitt went down hitting her head, but as I started to approach her, she jumped up and continued playing. I keep a close eye of her and every couple minutes she would touch her head, but would not come out. After the game she came up to me and explained she had a headache and felt like she was in a daze but did not want to come off the field during the game. I looked at her eyes and there was some nystagmus. I told her to avoid anything that worsens symptoms, so if light was bothering her to stay away from her phone and rest.
Earlier in the week I was able to take out one of my rugby players stitches from a rugby match two weeks prior. The wound was healing nicely, and the scab looked great, so Joe and I felt good about take out his stitches. So, I was able to remove his stitches without a problem and have him practice Thursday. I was hesitant to having him play in the game Saturday, but he had sat out for two weeks and was ready to get going again. I padded him up really good and keep it clean, however during the first half I noticed blood coming through the gauze, I checked on him, but he claimed he was okay and kept playing. Then about half way through the first half a VMI player come up to me complaining of posterior shoulder pain, while I accessed range of motion his right arm was only able to get about half way compared bilaterally and strength was about the same. He was pretty weak and very tender on the posterior shoulder muscles. I decided a posterior subluxation while playing most likely happened. I created a sling with his sweatpants and put ice on his shoulder. I checked on him a couple times throughout the game, but he seemed be doing well. Near the end of the second half my player went down and when getting up seemed to be in pain on his right shoulder and had a large amount of blood in the gauze on his knee now. I ran up to him and as I was walking up the game ended, I peeled off half of the gauze and noticed the scab was non-existent and the cut was completely reopened. Joe and I started to go through options in our heads and then the coach said his friend that is an anesthesiologist was at the game. We walked over to him and he confirmed the he cannot be re-sutured so keep it clean, antibiotic ointment, covered, butterflied and allow it to heal on its own. On Sunday I passed my practice BOC exam, so I will be able to sit in the March/April window! |


 RSS Feed
RSS Feed
